Main Second Level Navigation
Breadcrumbs
- Home
- News & Events
- Recent News
- A Glimpse into Future of Medicine at UofTMed Student Showcase
A Glimpse into Future of Medicine at UofTMed Student Showcase

Carolyn Morris
 Second-year medical student Corey Sermer knows first-hand how debilitating joint pain can be. His knees are increasingly stiff and swollen, as the cartilage continues to degenerate due to sports injuries. He’s had several operations so far and will be undergoing another this June.
Second-year medical student Corey Sermer knows first-hand how debilitating joint pain can be. His knees are increasingly stiff and swollen, as the cartilage continues to degenerate due to sports injuries. He’s had several operations so far and will be undergoing another this June.
This makes him especially keen on a new biological joint replacement for osteoarthritis that he’s helping to develop — it’s something he might need himself down the line.
In Laboratory Medicine and Pathobiology Professor Rita Kandel’s lab, and in collaboration with orthopaedic surgery lecturer Dr. John Theodoropoulos, Sermer is growing biological tissue to repair damaged cartilage.
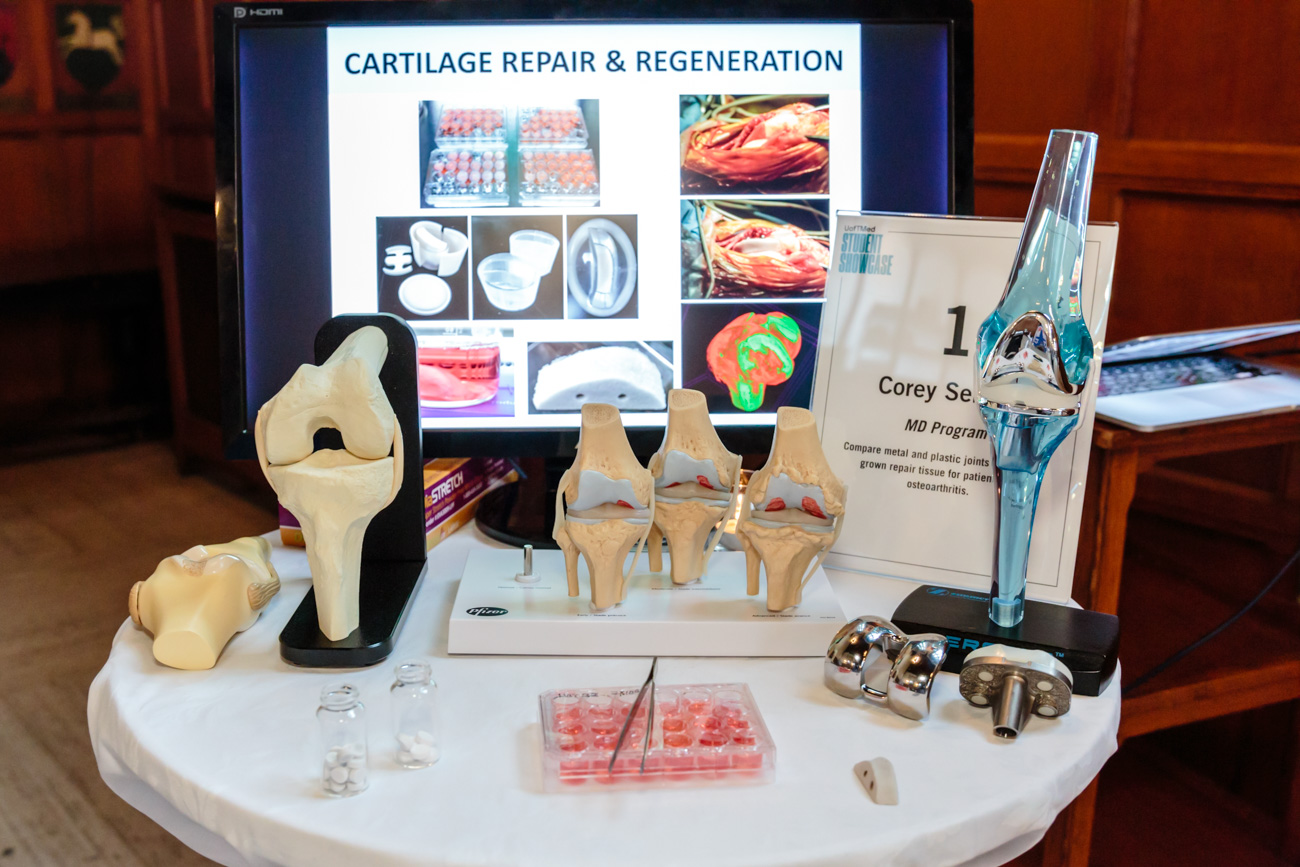
“Instead of a large metal bone replacement, we create a porous 3D-printed bone substitute. Then we grow real cartilage to line it, before inserting it during surgery,” he explains. “As opposed to metal and plastic, these biological materials can really blend into our bodies. Our bone will grow into the replacement over time, and the lab-grown cartilage will provide real cushioning.”
Sermer's project was one of 15 on display this week, at a donor-focused event called UofTMed Student Showcase — and it won the event’s Donor’s Choice Award.
“We often talk about the programs or projects that are made possible by philanthropic donations,” said Dean Trevor Young, “we talk a little less about the people — about the students and trainees who are given the opportunity to focus their talent and knowledge.”
The evening was brimming with talent and knowledge from learners across the Faculty, and across disciplines.
Vascular surgery resident Patrick McVeigh showed how a vascular endoscopy outfitted with a miniature camera could improve the accuracy of blood vessel stenting. Rehabilitation sciences PhD candidate Lucas Crosby made the connection between music and symmetrical walking for stroke recovery. Medical student Nicholas Sequeira measured attendees’ heart function with a wearable device that could potentially track long-term health of patients at risk of heart disease.
“This is such a unique chance to delve into some of the innovative research and technologies our students are involved in,” said Darina Landa, executive director of the Faculty’s Office of Advancement. “And as valued supporters of the Faculty, you are investing in health-care’s future leaders.”
Graduating medical student Brad Weston spoke about the impact donor support can have in opening new opportunities for learning. As a father with three young children, he said financial support was critical in enabling him to focus on his training.
As for Sermer, who began working on lab-grown tissue repair during his master’s at the Faculty’s Institute of Medical Science, he hopes to continue this research throughout his MD program and foresees a career in surgery and tissue engineering research.
He would love to see the biological joint replacement surgery become available in five to ten years — hopefully long before he’ll ever need it.
 The 15 projects on display were:
The 15 projects on display were:
Lab-grown tissue for osteoarthritis repair: MD student Corey Sermer exhibited the future of joint surgery with 3D-printed bone and lab-grown cartilage from the Kandel Lab.
Microscopic camera tracks neuronal activity: Institute of Medical Science (IMS) fellow Chen Yan and psychology student Alex Jacob displayed footage from a tiny camera inside the brain of animal models, and how he tracks neuronal activity related to memory.
Blood vessel camera: Vascular surgery resident Patrick McVeigh demonstrated how a miniature camera attached to a blood vessel endoscopy can guide placement of a stent.
Aging simulation suit: Translational Research Program graduate students Catherine Rivers and Haley Roher gave attendees a chance to try out an aging simulation suit, which health care providers can use to develop empathy for patients.
Stem cells and spinal cord injuries: Neurosurgery resident Christopher Ahuja, with IMS and supervised by Surgery Professor Michael Fehlings, challenged attendees to simulate a stem-cell transplant by injecting dye into a 3D-printed spinal cord sample.
Physician wellbeing and mindfulness: IMS PhD candidate Elli Weisbaum led a guided mindfulness meditation and presented a meditation app.
Reframing disability among medical students as source of expertise: Medical student Erene Stergiopoulos invited attendees to explore how disabilities might be an advantage in providing compassionate health care.
LGBTQ+ and cookie decorating: Medical students Herman Tang, Kaiwen Song and Alex Coutin sparked conversation on sexual orientation and gender in medicine through a “genderbread person” decorating station.
Marketing sugary cereals to kids: Nutritional sciences master’s student Christine Mulligan showed which children’s cereals would not be allowed under a proposed Health Canada nutrient profiling model.
Wearable device to measure ECG: Medical student Nicholas Sequeira showed how a wearable device could track long-term health of patients at risk of heart disease.
Eye and ear simulation helps students hone skills: Medical students Mirriam Mikhail and Stephen Szeto show how OtoSim and Ophthosim help health care students and professionals practice identifying early signs of hearing and vision problems.
Nature via virtual reality for patients with dementia: Medical student Orly Bogler invited attendees into a virtual world of nature. She is involved in research on the benefits of this immersive activity among patients with dementia.
Quick and customized 3D-printed finger casts: An MD student pairing his full-time medical education with a part-time master’s of engineering, Jason Jaewoo Park made on-the-spot 3D-printed finger splints for attendees — something he worked on with the Toronto-based company 3D4MD, aimed at making low-cost medical items in low resource settings.
Aortic aneurysm repair: Medical students Helen Genis and Sean Crawford challenged attendees to try out a simulated minimally invasive surgery to repair aortic aneurysm. As part of their summer research program with Surgery Professor Thomas Forbes, they use computer models to improve this technique.
Music, walking and stroke recovery: Rehabilitation sciences PhD candidate Lucas Crosby connected the dots between rhythm, gait and recovery from stroke — and discussed his research with supervisor Professor Kara Patterson.

News


